ML Claim
General Liability and Worker’s Comp Claim Predictor

The only GL Claim predictor in the market & we do Worker’s Comp too.
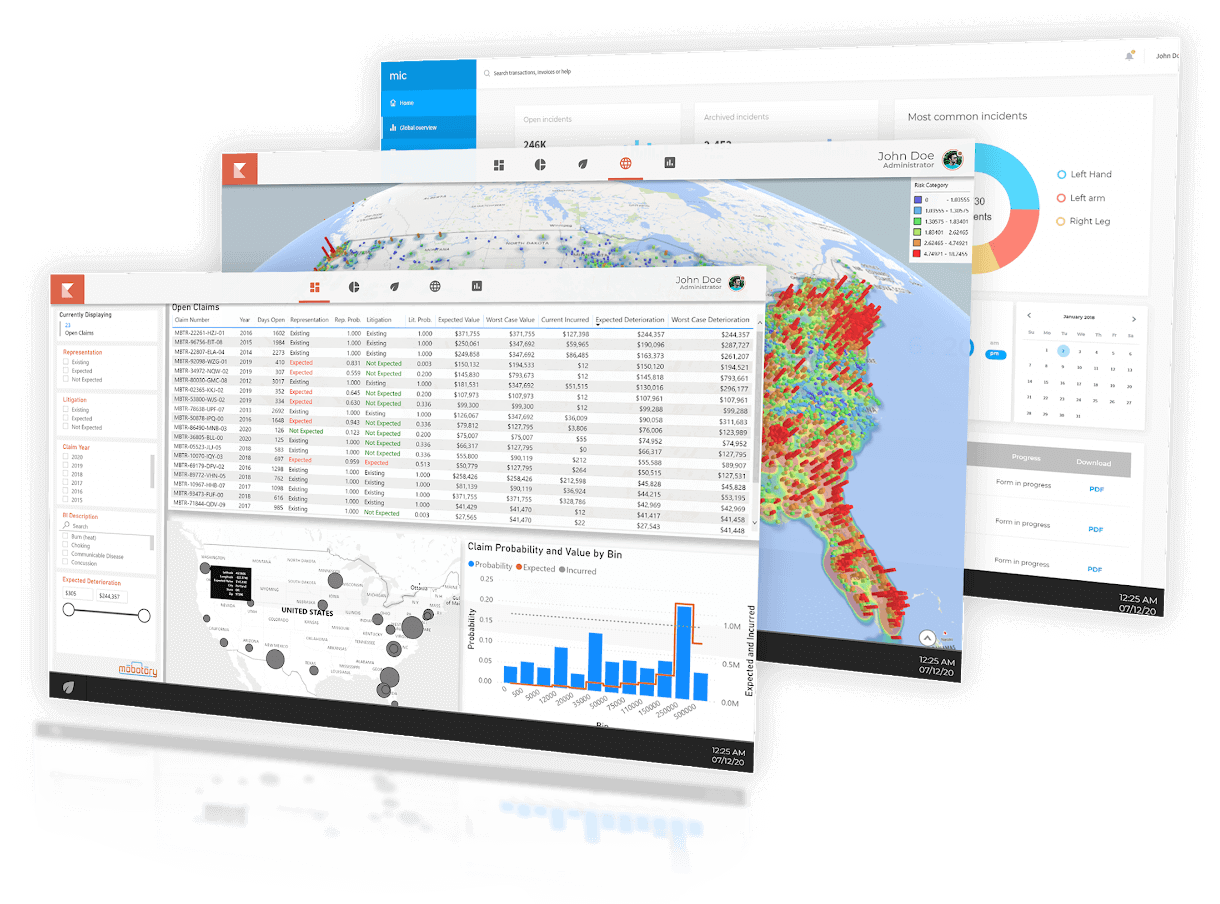
Key benefits
· Produce better loss ratios
· Faster settlements by forecasting issues & costs
· Reduce unnecessary payment of future claims
· Shortens the life of claims
Dashboard management
· Quick access KPIs
· Data visualization
· Trends in claims
· Predefined Insights
· Historical comparison
Alert system
· Early adjuster alerts of claims with the potential for high leakage
· Custom alerts to help your team in the claims handling process
It’s Fast
· Receive predictions within 48 hours when a new claim is filed
· Automatically updates probabilities as data and claim condition changes
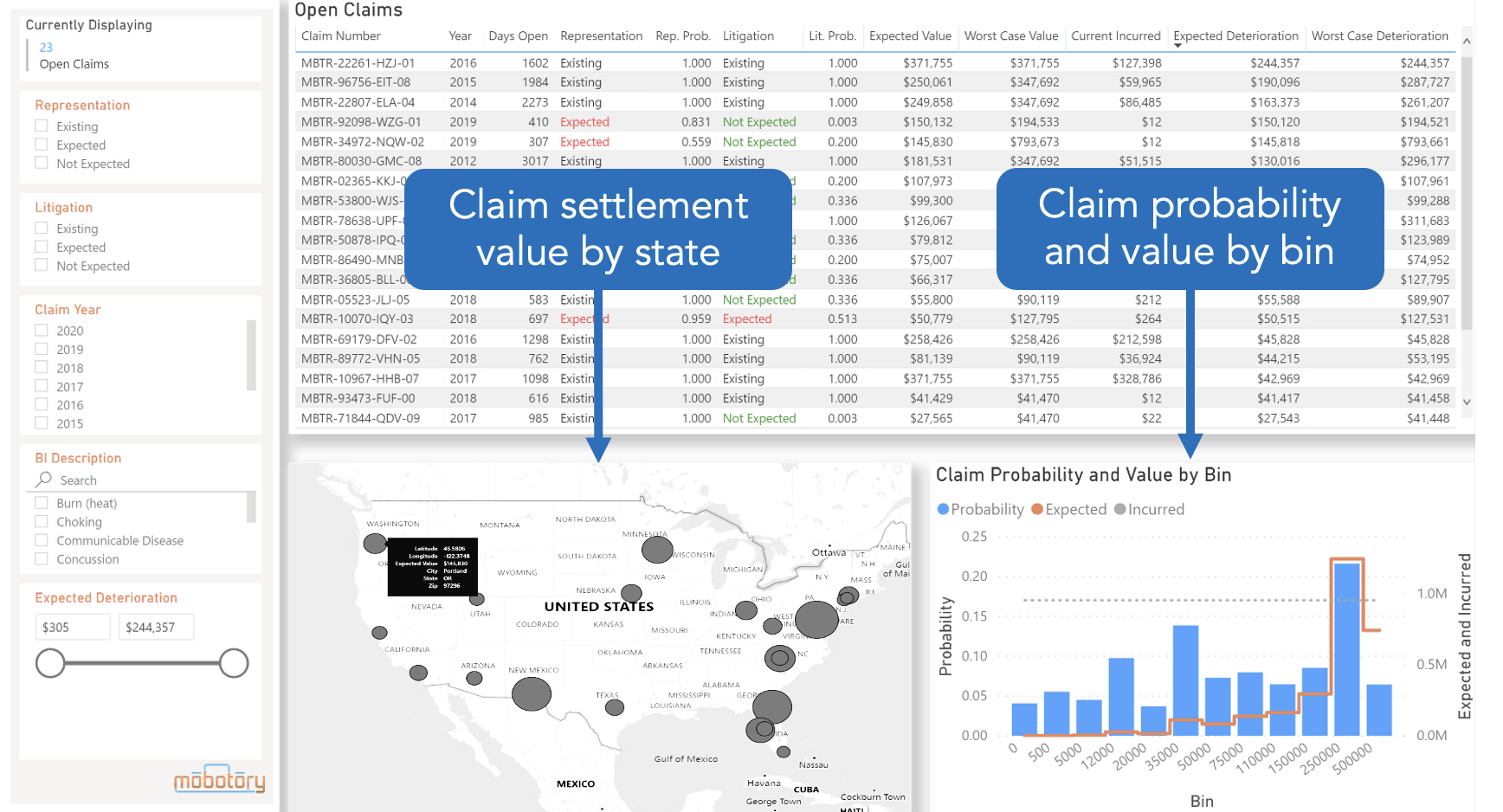
AI + BI = Predictive Analytics
We use the combination of Artificial Intelligence and our Business Intelligence to form robust predictive analytics on Workers’ Comp and General Liability Claims. Our Core engine is able to uncover complex patterns, trends, and correlations that otherwise would go unnoticed. Our Claims Predictor gives claims specialist, TPA’s, and other stakeholders in the claims lifecycle process the tools and insights they need to reduce the overall claim cost for their organization.
 
How it Works
Our Claims Predictor connects directly to your internal data sources, integrates it with applicable external third-party data, and crunches it through our core engine to discover hidden correlations that show the true nature of the claim. In real-time, as a claim is reported, our platform automatically flags the claims that are problematic.
At 90% accuracy, the Claims Predictor predicts the probability a claimant will solicit legal representation and the probability the claim will move into litigation. A cost prediction benchmark updates as conditions of the claim evolve. This allows cost containment efforts to be applied to problematic claims starting day 1 of the claim.
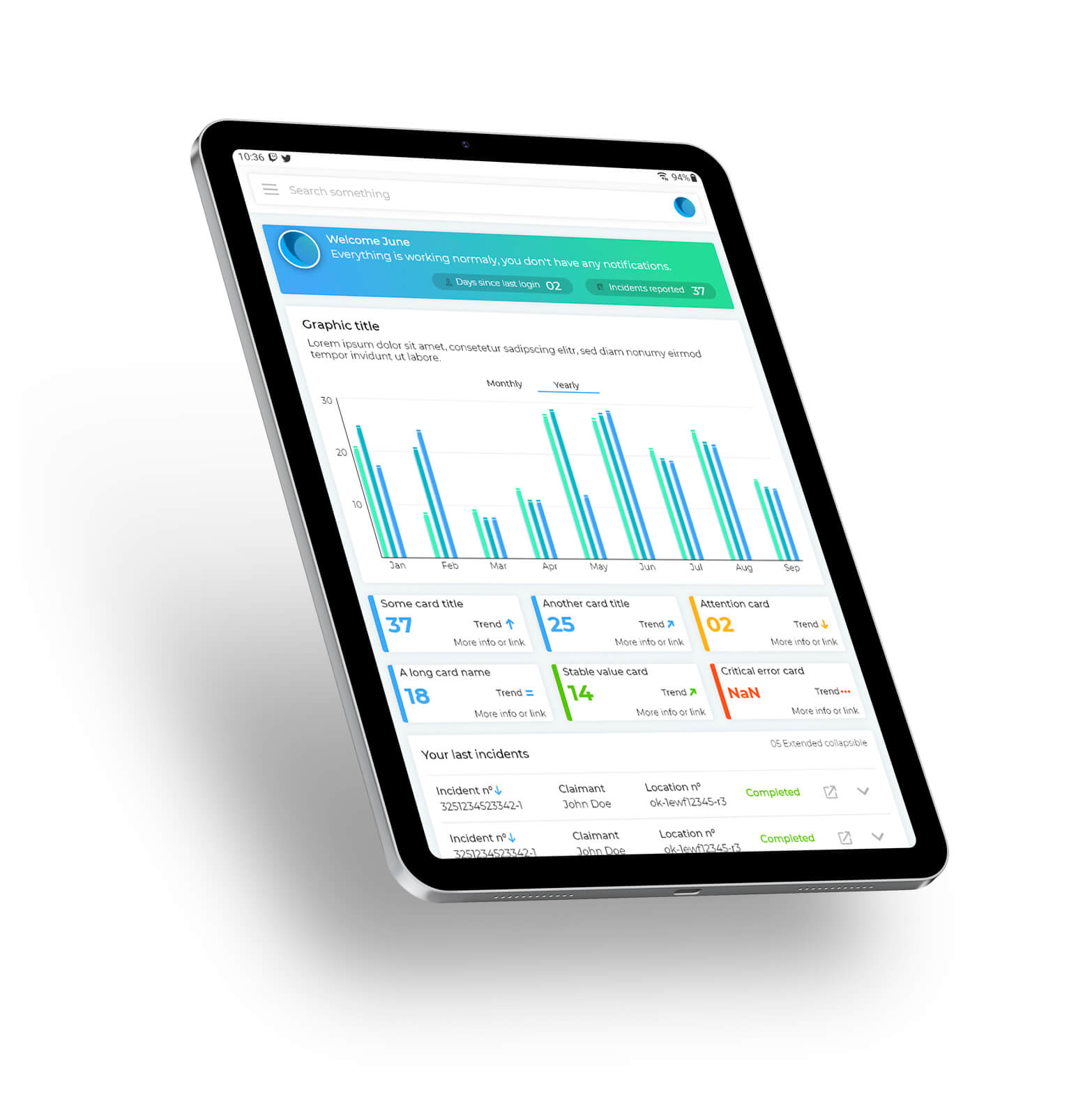
ML Intake
Combining the claims predictor with our mobile in-field reporting apps, ML Intake & ML Track, feeds clean data straight into our engine, bringing even more accurate results. Our mobile apps also arm you with a full digital defense file.
